How Can International Partners Help China’s Goal to Eliminate Hepatitis C in Nine Years?

March 23, 2021 | By Zixiang (George) Zhou, Associate, Bridge Consulting | Image source: MSF Access Campaign
March 18, 2021 marked China’s 21st National Protect Your Liver Day. In 2016, the WHO adopted the Global Health Sector Strategy on Viral Hepatitis, an action plan to end viral hepatitis as a major public health risk by 2030, and China has committed itself to meet that goal. China has the world’s largest burden of hepatitis B virus (HBV) and hepatitis C virus (HCV) infections. Although China has made significant progress in combating hepatitis B in the past decades, its fight against hepatitis C has been less successful. With only nine years left for China to achieve elimination of viral hepatitis as a public health risk and facing many challenges, stakeholders in China need to take more action to fight hepatitis C and international partners can aid their efforts.
Hepatitis C in China
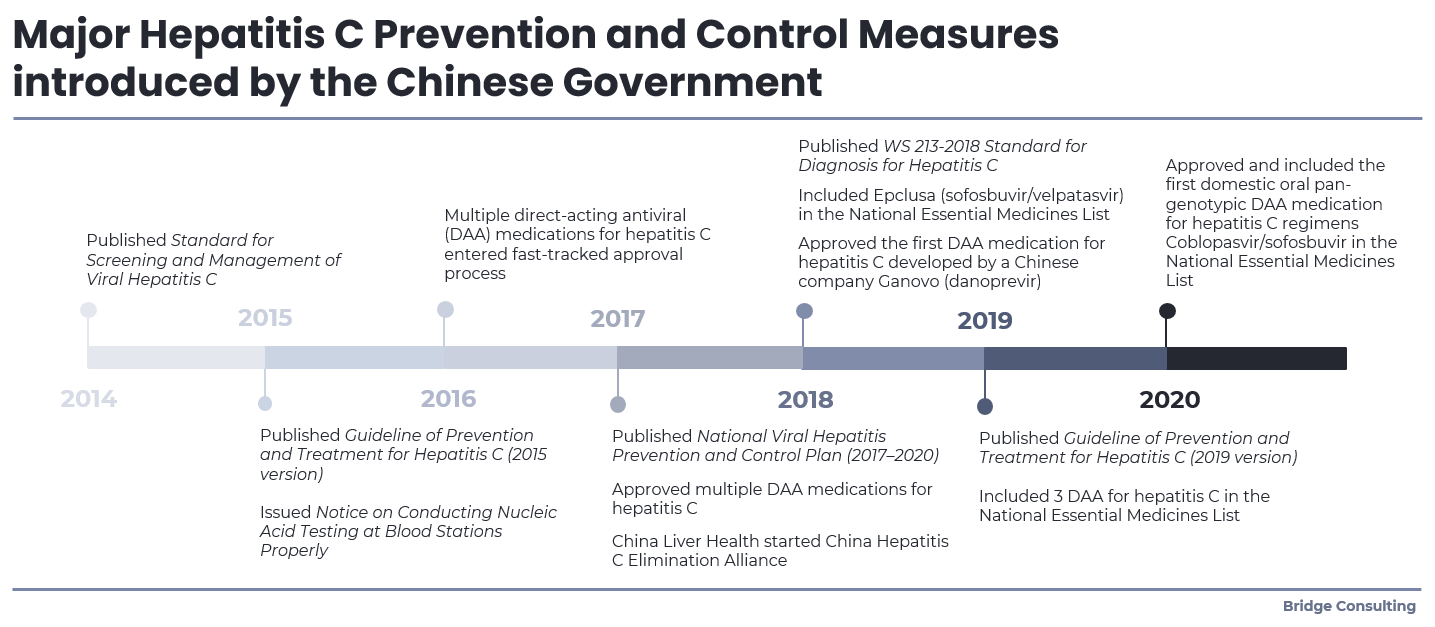
Estimations of people infected with HCV in China vary, ranging from 7.6 to 10 million. While China has made progress controlling hepatitis C through measures and accelerated efforts since committing to WHO’s elimination goal set in 2016 (see Figure 1), significant challenges remain. A Chinese expert noted in July 2020 that the diagnostic rate of hepatitis C is only 2 percent while the antiviral treatment rate for hepatitis C patients is below 1 percent. China’s effort to combat hepatitis C continues to be hampered by several issues, including:
Low Public Awareness. According to a survey conducted by the Chinese Foundation for Hepatitis Prevention and Control in recent years, only 38 percent of respondents have heard of hepatitis C, compared to 91 percent for hepatitis A and 95 percent for hepatitis B. Because of low public awareness, many HCV carriers are not aware of their condition.
Limited Access to Screening. Experts noted that screening at lower-tier hospitals, especially those in less developed and rural areas, remains weak. Many lower-tier hospitals at the county level cannot conduct nucleic acid testing and patients may need to travel to higher-tier hospitals far away from them in order to get tested. This severely limits HCV screening in these areas.
Limited Access to Treatment. HCV treatment was very expensive for many patients in China. A state media report in 2018 described how patients had to purchase imported generic drugs through illegal, underground channels at the risk of purchasing fake drugs because they could not afford the much more expensive version available through legitimate channels and there was no cheaper alternative. Although several hepatitis C regimens have been added to the National Essential Medicines List since 2019, experts reported that these newly listed drugs are still not available at many lower-tier hospitals, especially those in remote areas. Some patients still have difficulties getting reimbursed for these newly listed hepatitis C drugs due to issues with regional medical insurance policies.
Fragmented Governance System. Currently viral hepatitis control in China is managed by different departments of China’s National Health Commission (NHC) based on the transmission patterns or control strategies of other diseases. HBV prevention is led by the Division of Immunization Planning Management while HCV prevention is led by the Division of HIV/ AIDS Prevention and Control. A 2020 report by Duke University and the Development Research Center of the State Council of China pointed out that this has caused “a lack of central strategic planning and leadership, which has further led to inadequate financial and personnel support.” According to the same report, hepatitis C control in China is also highly dependent on the work plan, budget, skills and personnel for HIV/AIDS.
Other Issues. Discrimination, social stigma and legal issues prevent adoption of harm reduction practices to prevent HCV infections among drug users. Other high-risk groups such as men who have sex with men also suffer from discrimination and social stigma in China. Non-standardized treatment given to patients is also an issue. Sometimes overtreatment is given to diagnosed hepatitis C patients by doctors in order to generate income. Inadequate awareness and capacity at lower-tier hospitals could also result in skipped testing, incorrect diagnosis, and hospital-acquired infection.
What China Has Done in Recent Years to Address these Problems?
In the face of these issues and challenges, various stakeholders in China have been taking action to improve the situation.
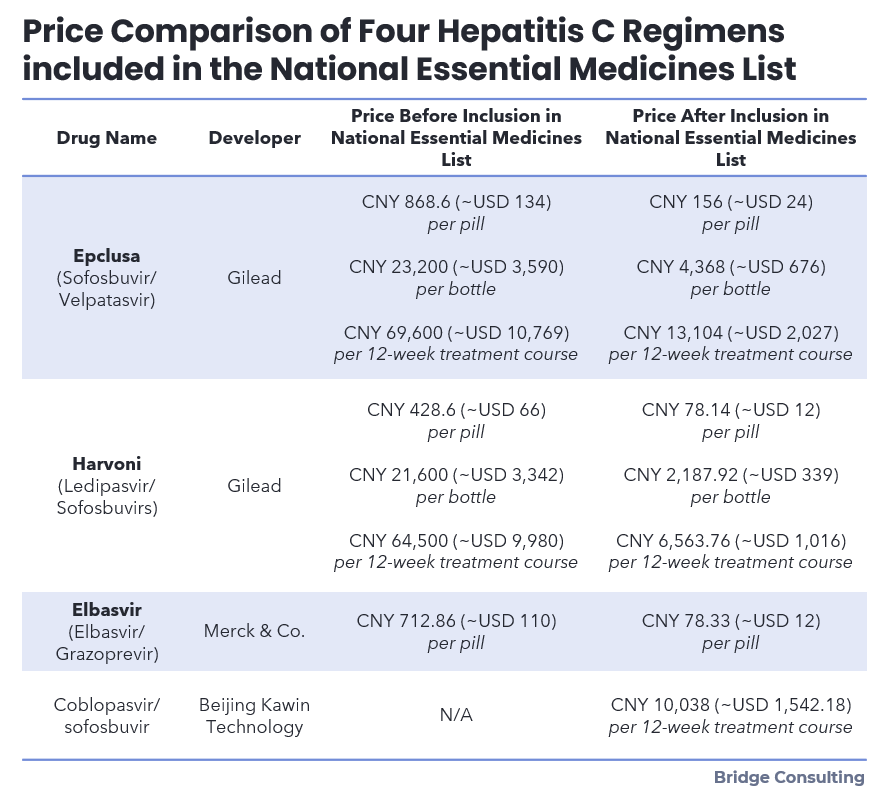
Increase Access to Treatment. After tough negotiations in 2019, China announced the inclusion of three hepatitis C regimens, Epclusa, Harvoni and Zepatier in the National Essential Medicines List starting in 2020, which opened the door for these drugs to become publicly funded under China’s public health insurance programs. Their prices were slashed by more than 85 percent. Another affordable domestic alternative coblopasvir/sofosbuvir combination developed by Beijing Kawin Technology was also approved and included in China’s National Essential Medicines List in 2020. (See Figure 2) New medical insurance policies were also adopted by some regions which have greatly reduced the cost of hepatitis C treatment. For example, in Hunan province, medical insurance can cover up to 80% of the cost of hepatitis C treatment, greatly relieving the financial burden on patients.
Increase Access to Screening. China has been investing in its nucleic acid testing capacity. The COVID-19 pandemic prompted further investment in this capacity by the central and local governments as part of their efforts to improve their overall public health system. A government official noted that China can test more than 16 million samples per day as of February 1, 2021, compared to 1.26 million samples per day in March 2020. Increased nucleic acid testing capacity across China will no doubt increase access to hepatitis C screening.
Raise Public Awareness. Stakeholders in China have been working to raise public awareness of hepatitis C. Government agencies such as the National Health Commission and domestic civil organizations such as the Chinese Foundation for Hepatitis Prevention and Control and China Liver Health have been using opportunities such as the National Your Protect Liver Day and World Hepatitis Day to educate the public on hepatitis C.
Develop New Strategy. China has also been working on new strategies to fight the hepatitis C epidemic. In 2019, the city of Ningbo launched a 2019-2022 action plan that aims to eliminate hepatitis C as a public health risk, making it the first city in China to do so. Government agencies including the local health commission and medical insurance administration worked with civil organizations such as China Liver Health and implemented measures including strengthening public education, strengthening intervention measures to prevent infection, standardizing treatment and follow-up, and enhancing monitoring of the disease.
How Can International Partners Contribute?
Assisting China in its battle against hepatitis C can help the world meet WHO’s goal of eliminating viral hepatitis C by 2030 and advance the Sustainable Development Goal 3.3 of ending the epidemics of AIDS, tuberculosis, malaria and neglected tropical diseases and combating hepatitis, water-borne diseases and other communicable diseases by 2030. International stakeholders could contribute to China’s efforts in a number of ways:
Increase Access to Screening and Treatment. Although China has made a great effort to increase access to screening and treatment for hepatitis C patients, some gaps remain, and international partners could help China fill these gaps. WHO has estimated prices offered by suppliers of WHO-prequalified HCV rapid diagnostic tests to be between USD 1-8 per test. These could be very helpful especially in low-resource settings in remote and rural parts of China where hepatitis C screening rates remain low. The Drugs for Neglected Diseases Initiative (DNDi), a non-profit drug research and development organization, managed to bring down the cost of a new hepatitis C regimen (ravidasvir/sofosbuvir) to USD 300 per 12-week treatment course in Malaysia. This innovation has the potential to further increase access to treatment by hepatitis C patients in China if DNDi can introduce it into the Chinese market.
Improve Eradication Strategy. International partners can also help China to review its hepatitis C fighting strategy and governance apparatus and give recommendations based on their evaluation and experience. For example, the Bill & Melinda Gates Foundation funded a report on China’s efforts to combat hepatitis B and C. This study jointly conducted by international partners such as the Duke Global Health Institute and Chinese stakeholders such as the Development and Research Center of State Council thoroughly examined the gaps and challenges in hepatitis B and C control in China and proposed practical recommendations.
Raise Public Awareness. International organizations can also use their platforms or work with Chinese stakeholders to raise public awareness of hepatitis C. Over the past years, WHO’s China office has launched several communications campaigns to raise public awareness on viral hepatitis-related issues on World Hepatitis Day. The Bill & Melinda Gates Foundation has also published articles on hepatitis C on its Chinese social media channels to offer the Chinese public more information on this topic.
Develop Better Projects. International organizations can also share their experience in combating hepatitis C and other know-how with the Chinese stakeholders by helping China develop better hepatitis C control project. For example, Médecins Sans Frontières (MSF) designed a model of cooperation with the Ukrainian Ministry of Health to use generic drugs to treat hepatitis C in Ukraine. In this project, MSF provided all the supplies including medications, the tests, and laboratory equipment as well as other services such as mental health support for patients, and it fully handed over the project to local health authorities after its goals were achieved.
China’s fight against hepatitis C is closely linked with the world’s effort to control viral hepatitis. The COVID-19 pandemic again showcases the need for international cooperation in controlling infectious diseases in the highly connected world today. China has indeed made significant progress in fighting viral hepatitis, especially hepatitis B, but controlling hepatitis C remains a weak point. By joining forces with stakeholders in China to control hepatitis C, international stakeholders can contribute greatly to the global goal of ending viral hepatitis by 2030.
About The Author
Zixiang (George) Zhou
Zixiang (George) Zhou is an experienced international relations and development professional who has worked in Washington DC, Nairobi, and Beijing. Find George on LinkedIn.